You look in the mirror and see a red, itchy patch on your skin. It’s uncomfortable, maybe even painful, but here is the tricky part: is it eczema or psoriasis? You aren't alone in wondering this. In fact, a 2022 study in the *Journal of the American Academy of Dermatology* found that misdiagnosis happens in 15-20% of cases. Why does this matter? Because treating one like the other can make things worse. While both are chronic inflammatory skin conditions, they have distinct visual signatures if you know where to look.
Getting the diagnosis right isn't just about vanity; it's about effective treatment. Eczema, formally known as atopic dermatitis, is an immune-mediated reaction often triggered by irritants. Psoriasis, on the other hand, is an autoimmune disorder that speeds up skin cell production. Understanding the visual differences helps you communicate better with your doctor and manage your skin more effectively.
The Location Test: Inside vs. Outside the Creases
The first clue usually lies in where the rash appears. This is often the most reliable differentiator before you even look closely at the texture.
Eczema is a condition that predominantly affects flexural surfaces-the inner folds of the body. According to a 2021 clinical review in *Dermatology Practical & Conceptual*, 92% of eczema cases appear on the inner elbows, and 89% appear behind the knees. If you are looking at a baby, check the cheeks (76% of pediatric cases) and wrists. The rule of thumb? Eczema likes the "inside" of the joints.
In contrast, Psoriasis favors extensor surfaces-the outer parts of the joints. Dr. Peter Lio from Northwestern University notes that psoriasis typically shows up on the outer elbows (85% of cases), the front of the knees (78%), the scalp (80%), and the lower back. A 2020 *JAMA Dermatology* study confirmed this pattern: 88.6% of psoriasis cases affected extensor surfaces, compared to only 9.1% for eczema.
| Body Area | More Likely Eczema | More Likely Psoriasis |
|---|---|---|
| Elbows | Inner crease (92%) | Outer surface (85%) |
| Knees | Behind the knee (89%) | Front of the knee (78%) |
| Scalp | Rarely primary site | Very common (80%) |
| Face | Cheeks (especially infants) | Hairline and eyebrows |
| Nails | Rare involvement (5-10%) | Frequent pitting/separation (50-80%) |
Visual Morphology: Borders and Scales
Once you’ve checked the location, look at the shape and texture of the rash itself. The way the skin looks under close inspection tells a very different story for each condition.
Eczema rashes are often poorly defined. They don’t have sharp borders; instead, they blend into the surrounding normal skin. On lighter skin tones (Fitzpatrick I-III), eczema appears as red, inflamed patches. However, research in the *Journal of Investigative Dermatology* (2021) highlights that on medium to dark skin tones (Fitzpatrick IV-VI), eczema may present as ashen, purple, or gray patches. The texture is usually thinner, and in acute phases, it might weep, crust, or ooze fluid. Chronic scratching leads to lichenification, where the skin becomes thickened and leathery, but this is a result of damage, not the initial plaque formation.
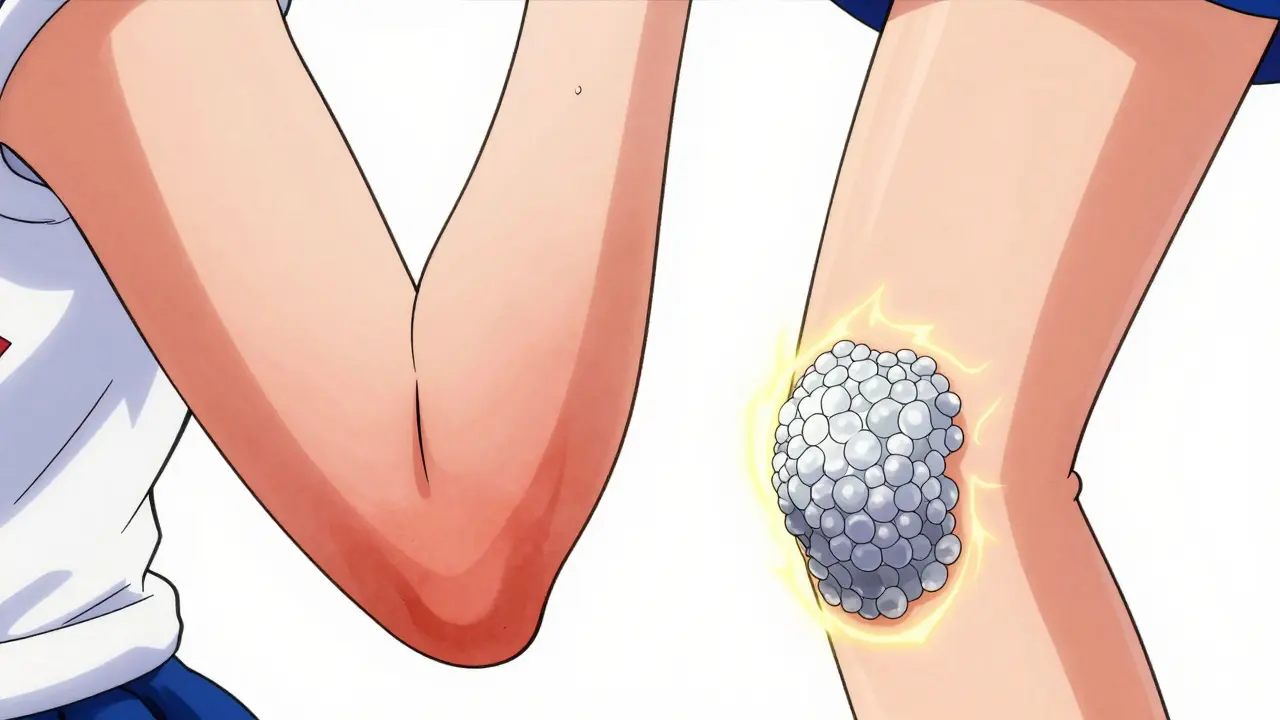
Psoriasis presents differently. It features well-demarcated, raised plaques with thick, adherent silvery-white scales. These lesions stand out clearly against the surrounding skin. On darker skin tones, psoriasis appears as violet, dark brown, or ashen patches, but the silvery scale remains a key identifier. A 2023 *British Journal of Dermatology* study found that 78% of psoriasis lesions exhibited visible scaling, compared to only 32% of eczema lesions. Furthermore, psoriasis scales are significantly thicker-averaging 0.5mm versus 0.1mm for eczema.
Here is a practical test recommended by the Mayo Clinic: gently scrape the lesion with a glass slide or fingernail. If thick, silvery scales come off easily and reveal pinpoint bleeding underneath (known as the Auspitz sign), it is likely psoriasis. Eczema scaling is finer and does not bleed when removed.
Nail Changes and Skin Surface Texture
If the rash is hard to distinguish, look at your nails. Nail involvement is a strong indicator for psoriasis and rarely occurs in eczema.
In psoriasis, nail changes are common. About 50% of patients experience nail pitting-small depressions in the nail plate. Additionally, 80% of those with nail involvement show onycholysis, which is the separation of the nail from the nail bed. The nail may also become thickened or discolored yellow-brown.
Eczema rarely affects the nails. When it does, it’s usually limited to mild ridging or discoloration in severe cases, but true pitting is absent. Another visual clue is the Koebner phenomenon. In 25-30% of psoriasis patients, new lesions form at sites of skin trauma, such as cuts or scratches. This is rare in eczema. So, if you notice a new patch forming exactly where you scraped your elbow last week, think psoriasis.
Differences in Skin of Color
Traditional medical textbooks often depict these conditions on lighter skin, which can lead to diagnostic delays for people with darker skin tones. The Skin of Color Society reports that misdiagnosis rates are 35% higher in patients with Fitzpatrick skin types IV-VI.
On darker skin, inflammation doesn't always look red. For eczema, look for hyperpigmented (darker) or hypopigmented (lighter) patches with subtle scaling. The lack of bright redness can make it harder to spot early signs. For psoriasis, the plaques often appear violaceous (purple) or dark brown. A landmark 2023 study in the *Journal of Investigative Dermatology* noted that psoriasis on darker skin frequently shows a characteristic 'halo' of hypopigmentation around active lesions in 68% of cases-a feature absent in eczema.
Dr. Jenna Lester from UCSF emphasizes that while the color changes, the structural differences remain. Psoriasis still has the thick, adherent scale and well-defined borders, while eczema remains poorly defined and prone to oozing or crusting. Being aware of these variations is crucial for accurate self-assessment and timely medical consultation.

Patient Perspectives and Daily Impact
Beyond clinical metrics, how patients describe their experience offers insight into the visual nature of these conditions. Data from the National Eczema Association forum shows that 87% of respondents describe eczema as "raw-looking, weepy skin that cracks and bleeds easily." It feels fragile and sensitive.
In contrast, users on the National Psoriasis Foundation forum (76%) characterize psoriasis as "thick, silvery patches that look like armor plating." It feels hard and scaly. Reddit discussions analyzed in 2024 reinforced this: 63% of eczema patients mentioned oozing and crusting as defining visuals, while 89% of psoriasis patients referenced thick, silvery scales. Patients with psoriasis were 3.2 times more likely to report their condition as "visually distinctive and immediately recognizable," whereas eczema patients described their rashes as blending into normal skin.
When to See a Doctor
While visual clues help, they aren't a substitute for professional diagnosis. Teledermatology tools have improved, with some AI classifiers achieving 85% accuracy, but the American Academy of Dermatology warns that no digital tool replaces a clinical exam, especially for skin of color where algorithmic bias persists.
Seek medical advice if:
- The rash covers a large area of your body.
- You experience severe itching that disrupts sleep or daily activities.
- The skin shows signs of infection (pus, warmth, fever).
- Over-the-counter treatments provide no relief after two weeks.
Early and accurate diagnosis ensures you get the right treatment plan, whether it involves topical steroids for eczema or biologics for psoriasis. Don't hesitate to ask your dermatologist specifically about the location and scale characteristics to ensure a thorough evaluation.
Can you have both eczema and psoriasis?
Yes, it is possible to have both conditions simultaneously, though it is rare. This is called comorbidity. If you have features of both, such as flexural eczema and extensor psoriasis, a dermatologist can diagnose both through clinical examination and possibly a skin biopsy.
What is the Auspitz sign?
The Auspitz sign is a clinical indicator of psoriasis. It refers to pinpoint bleeding that occurs when the thick, silvery scales of a psoriasis plaque are scraped off. This happens because the blood vessels in the papillary dermis are dilated and close to the surface. Eczema does not exhibit this sign.
How does eczema look on dark skin?
On darker skin tones, eczema may not appear red. Instead, it can present as ash-gray, purple, or brown patches. It often lacks the bright erythema seen on lighter skin. Look for poorly defined borders, dryness, and potential oozing or crusting. Hyperpigmentation or hypopigmentation may also occur after healing.
Is psoriasis contagious?
No, psoriasis is not contagious. It is an autoimmune disease caused by genetic and environmental factors, not by bacteria, viruses, or fungi. You cannot catch psoriasis from touching someone who has it or sharing personal items.
What triggers eczema flares?
Eczema flares are often triggered by external irritants such as soaps, detergents, wool, or synthetic fabrics. Allergens like dust mites, pet dander, or pollen can also cause reactions. Stress, humidity changes, and sweat are common internal and environmental triggers.
Can nail changes help diagnose psoriasis?
Yes, nail changes are a strong indicator of psoriasis. Pitting (small dents in the nail), onycholysis (separation from the nail bed), and thickening are common. Eczema rarely causes these specific nail changes, making them a useful diagnostic clue when skin rashes are ambiguous.

